Definition
Uveitis is a general term describing a group of inflammatory diseases that produces swelling and destroys eye tissues. These diseases can slightly reduce vision or lead to severe vision loss. The term “uveitis” is used because the diseases often affect a part of the eye called the uvea. Nevertheless, uveitis is not limited to the uvea. These diseases also affect the lens, retina, optic nerve, and vitreous, producing reduced vision or blindness.
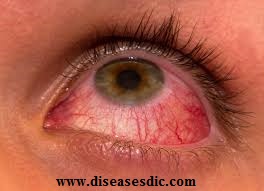
Uveitis
Uveitis may be caused by problems or diseases occurring in the eye or it can be part of an inflammatory disease affecting other parts of the body. It can happen at all ages and primarily affects people between 20-60 years old.
Types of Uveitis
There are several types.
Anterior uveitis
The most common type is inflammation of the iris, also known as iritis or anterior uveitis. A condition called iridocyclitis is similar, but it includes inflammation of the ciliary body.
Intermediate uveitis
Intermediate uveitis (vitritis) is an inflammation of the jelly-like part of the eye known as the vitreous cavity. A related condition is known as pars planitis, an inflammation of the pars plana, one of the eye’s layers.
Posterior uveitis
It is an inflammation of the retina and choroid at the back of the eye.
Pan-uveitis
It is an inflammation in all layers of the uvea.
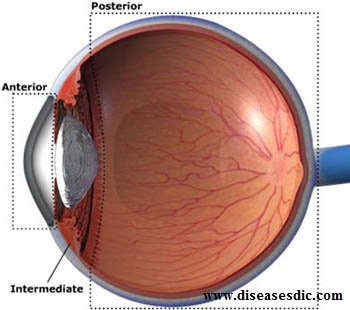
Types of uveitis
Risk factors
It is known that the following diseases can increase the risk:
Immune-mediated diseases
Immune-mediated diseases. Inflammatory bowel disease (Crohn’s disease, ulcerative colitis), juvenile idiopathic arthritis (JIA), spondyloarthropathies (ankylosing spondylitis, psoriatic arthritis, reactive arthritis), multiple sclerosis, etc.
Infected cell
Communicable diseases. Herpes, toxoplasmosis, tuberculosis, syphilis, HIV, Lyme disease, brucellosis, etc.
Severe traumatism in the eye
A history of severe eye trauma or previous eye surgery.
Types of cancer
Some types of cancer: lymphoma, leukaemia, melanoma, among others.
Causes of Uveitis
The cause of uveitis is often not clear but it can be caused by:
- Eye injury
- Eye surgery
- Autoimmune diseases
- Infection
- Cancer affecting the eye
- An inflammatory disorder, such as Crohn’s disease and ulcerative colitis
Symptoms
Symptoms include:
- Eye pain – usually a dull ache in or around your eye, which may be worse on focusing
- Eye redness
- Sensitivity to light (photophobia)
- Blurred or cloudy vision
- Small shapes moving across your field of vision (floaters)
- Loss of peripheral vision (the ability to see objects at the side of your field of vision)
The symptoms can develop suddenly or gradually over a few days. One or both eyes may be affected by uveitis.
Uveitis complications
If uveitis is untreated, uveitis can cause serious complications, including:
- Glaucoma
- Optic nerve damage
- Retinal detachment
- Cataracts
- Permanent vision loss
Diagnosis and test
Diagnosis comprises a thorough eye examination and the patient’s complete medical records. Lab tests may be conducted to rule out an infection or an autoimmune disorder.
The eye exams include:
An Eye Chart: This test measures whether a patient’s vision has decreased.
A Funduscopic Exam: The pupil of the eye is dilated with eye drops and then a light is shown through with an instrument designated an ophthalmoscope to noninvasively inspect the inside part of the eye.
Ocular Pressure: An instrument, such a tonometer, measures the pressure inside the eye. Drops that numb the eye may be used for this test.
A Slit Lamp Exam: A slit lamp noninvasively investigates the eye. It can examine the front and back parts of the eye and with a tonometer to measure eye pressure. A dye called fluorescein, which makes blood vessels easier to see, may be combined to the eye during the examination. The dye only temporarily stains the eye.
Treatment and medications
A patient with uveitis who receives prompt and appropriate treatment will usually recover. Without treatment, there is a risk of cataracts, glaucoma, band keratopathy, retinal edema, and permanent vision loss.
Antibiotics or antiviral medication will be used if there is an infection.
Corticosteroid medications are sometimes given as well, in the form of eye drops (prednisolone acetate), tablets, or as an injection into the eye. Steroids are effective in treating inflammation. Before giving corticosteroids, it Sis important rule out corneal ulcers by using a florescence dye test.
Immunosuppressants might be recommended if symptoms are very severe and there is a risk of vision loss, or if the patient has not responded well to other therapies.
Mydriatic eye drops such as atropine or cyclopentolate, dilate the pupil and help the eye to heal. It also helps with eye pain and stops the pupil from sticking to the lens. There may be blurred vision and unusual sensitivity to light, known as photophobia.
Eye drops for uveitis
Prevention
- Other than avoiding certain infections, including syphilis or HIV, there is no way to prevent uveitis.
- Seeking proper treatment for an autoimmune disease or infection can help to prevent uveitis. Otherwise healthy people is difficult to prevent since the cause isn’t known.
- Early detection and treatment are important to reduce the risk of vision loss, which can be permanent.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.




just waked up and find half my eye reddish what Could be the problem
Please consult a doctor to diagnose the problem.
How does the complications of uveitis com about???help me to explain how each complication is coming about
Please have a glance into the post regarding complications.
what advice would you give to a 30years old man who was born with red eye and had tried most doctors but could not get rid of it.
please help.
thanks
It might because of the genetic mutation that inherited.
I’m along sighted person but my left eye can not clearly only blurred vision
Kindly diagnosis with an ophthalmologist.
I am grateful to have your efforts (note kids). I enjoy it so much thank you once again for
why is it that my eyes redish are not paining me
It might be of inflammation of your eyes but it’s better to consult a doctor.
Can Macular disease be treated
without injection?. Please .
There’s no cure, but treatment for age-related macular degeneration (AMD) may slow the disease and keep you from having a severe loss of vision. Talk to your doctor about the best way to manage your condition.
Can someone with this problem use tuberculosis medication
No, they should not use unless or until they get a doctor’s prescription.