Overview
Phimosis is defined as the inability to retract the skin (foreskin or prepuce) covering the head (glans) of the penis. Phimosis may appear as a tight ring or “rubber band” of foreskin around the tip of the penis, preventing full retraction.
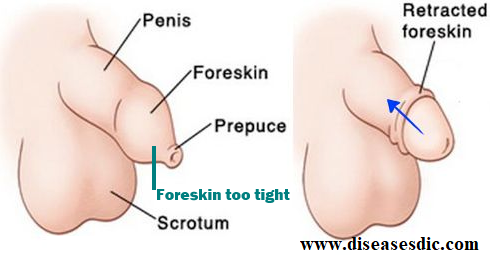
Types of Phimosis
Phimosis is divided into two forms: physiologic and pathologic.
Physiologic phimosis: Children are born with tight foreskin at birth and separation occurs naturally over time. Phimosis is normal for the uncircumcised infant/child and usually resolves around 5-7 years of age, however the child may be older.
Pathologic phimosis: Phimosis that occurs due to scarring, infection or inflammation. Forceful foreskin retraction can lead to bleeding, scarring, and psychological trauma for the child and parent. If there is ballooning of the foreskin during urination, difficulty with urination, or infection, then treatment may be warranted.
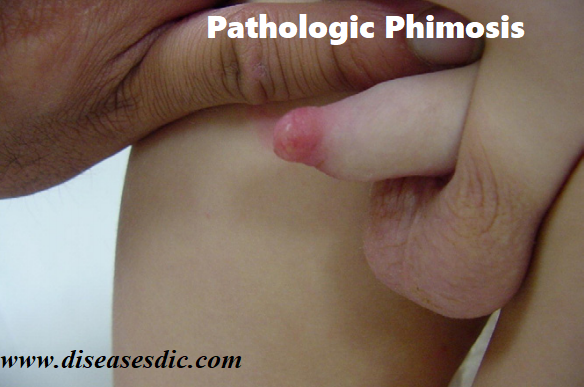
Pathophysiology
Retraction of the foreskin behind the glans penis (in the presence of a phimotic foreskin) leads to the phimotic ring causing constriction of the distal glans. This leads to vascular engorgement as the lymphatic and venous flow from the constricting ring are impaired. This results in secondary edema. The consequences are further vascular compromise as the arterial flow is impaired, and potential ischemia of the penis distal to the phimotic ring. Eventual necrosis of the glans penis may be observed. In other cases, the skin of the glans becomes thickened and dry, which leads to the chronic form of paraphimosis.
Causes and Risk factors
Phimosis only affects uncircumcised males and is more common in boys than men.
Phimosis is normal in uncircumcised babies and toddlers, as the foreskin is still attached to the glans. It will start to detach naturally between 2 and 6 years of age, though it might happen later. It can happen at up to around 10 years old, in some boys.
The foreskin can be pulled back behind the glans in about 50 percent of 1-year-old boys, and almost 90 percent of 3-year-olds. Phimosis will occur in less than 1 percent of teenagers between 16 and 18.
It is most likely to occur in older boys with:
- Repeated urinary tract infections
- Foreskin infection
- Repeated rough handling of the foreskin
- Foreskin trauma
In adults, risk factors for phimosis include sexually transmitted infections.
Phimosis may be caused by a skin condition, such as:
- Eczema: A long-term condition that causes the skin to become itchy, red, dry, and cracked.
- Psoriasis: This skin condition leads to patches of skin becoming red, flaky, and crusty.
- Lichen planus: An itchy rash that can affect different areas of the body. It is not contagious.
- Lichen sclerosus: This condition causes scarring on the foreskin that can lead to phimosis. It may be caused by a urinary irritation.
Signs and Symptoms
Symptoms of phimosis may vary in severity among affected individuals.
Common symptoms of phimosis include:
- Bulging of the foreskin (especially during urination)
- Difficulty urinating
- Inability to pull back the foreskin
- Pain
- Swelling of the tip of the penis
Symptoms that might indicate a serious condition
Paraphimosis is a serious condition that should be immediately evaluated in an emergency setting. Seek immediate medical care if you, or someone you are with, have any of these serious symptoms including:
- Discoloration or bruising of the penis tip
- High fever (higher than 101 degrees Fahrenheit)
- Inability to reposition the foreskin to the unretracted state
- Inability to urinate
- Tenderness around the scrotum
What are the Complications of Phimosis?
Though most of the cases of Phimosis go unnoticed, the condition might sometimes interfere with normal activities including:
- Painful or difficulty in urinating
- Difficult erections
- Swelling or inflammation of the fore skin
- Individuals may have severe stress and anxiety issues
- Forcible retraction of the skin can cause bleeding, pain, and scarring of the tissue, which makes the condition worse
- Discomfort and pain during sex
- Serious complications can lead to a condition called paraphimosis, which is the fixed retraction of the penile foreskin.
Diagnosis and Test
A physical examination of the penis and foreskin should suffice to diagnose a tight foreskin. Sometimes non retractibility could be due to a short penile frenulum (an elastic band of tissue that is connected to the foreskin and helps it to contract over the glans).
Doctors might question whether the penis has had any injuries or infections in the past or if the tight foreskin has affected sexual activity.
Other tests might be suggested in specific conditions. Examples are urine test and general blood test to exclude infection and to test for the presence of glucose (sugar). A swab from the foreskin area to check bacterial culture might also be taken.
Treatment and Medications
Medical opinion differs on the condition and on treatment of phimosis. It has been suggested that any radical or surgical treatments for phimosis should not be done until after puberty. This is partly due to a perception of overuse of circumcision as a mainstream treatment for phimosis.
If treatment is required there are three main types:
- Tropical creams, steroidal and non-steroidal, applied to the prepuce.
- Gradual stretching of the opening of the prepuce to widen it.
- Surgical reshaping of the prepuce to make it wider.
All these treatments tend to avoid the side effects associated with surgical circumcision, trauma, pain, side effects of removal of the foreskin such as friction and interference of the erogenous and sexual functions
Steroid creams – these may help to soften the skin and make it easier to stretch the foreskin. Usually, they are applied twice a day to the tip of the foreskin, for a period of four to eight weeks.
What to expect with steroid creams – after two weeks, you should be able to start gradually stretching the foreskin once a day. You should only do this after being shown how by a doctor. You should do this gently to avoid damaging the foreskin. Research has shown that this form of treatment is often successful at first. For example, one study showed that the use of a steroid cream in children was 84% successful. However, the use of a steroid cream often needs to be repeated and is not always a permanent solution.
Full circumcision – this a procedure where the foreskin is surgically removed, has become popular for the treatment of phimosis, particularly if the condition is caused by scarring. However, it can cause bleeding or lead to infections. It is usually considered as a last resort but may often be the most effective treatment option.
How does circumcision work? – Circumcision is carried out under general anaesthetic, but in some cases may be able to be performed under local anaesthetic instead. Men are often worried that the procedure will mean they won’t be able to feel much during sexual intercourse. However, many studies have shown that circumcision doesn’t affect sexual satisfaction. Possible complications of circumcision, include:
- Bruising
- Bleeding
- Wound infection
- Scar tissue
Partial circumcision – this has recently been shown to be an effective method for the treatment of phimosis. Plus, some people find it cosmetically more favourable as it almost completely preserves the foreskin. The procedure usually works the first time and only needs to be redone for 3.3% of people. It is also safe and simple.
In men who have had a complete circumcision, there is often a complaint of dryness and preservation of the foreskin prevents this. Therefore, partial circumcision helps to prevent this problem.
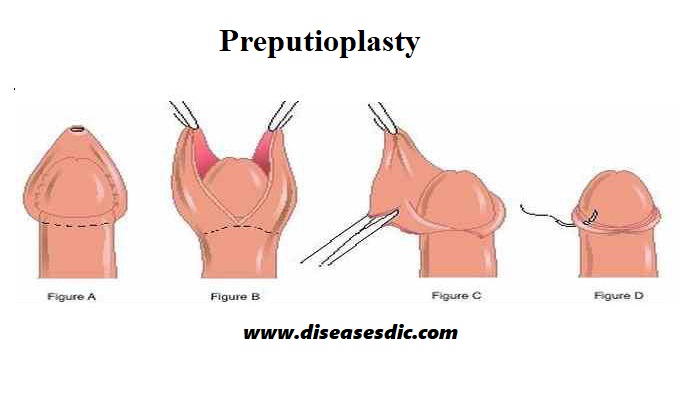
Preputioplasty – this is a less radical procedure compared to circumcision and may be more beneficial in children. The procedure involves making incisions at the tip of the foreskin, exposing the head of the penis. However, the procedure has little success in adults.
Home Remedies for Phimosis
- Practice Phimosis-stretching exercises
- Apply Chamomile cream
- Ayurvedic ointments might also help
How to prevent Phimosis?
Currently, there are no specific methods or guidelines to prevent Phimosis. However, the following factors may be considered:
- Gently wash your penis with warm water each day while having a bath or shower
- Gently pull back your foreskin (if you have one) and wash underneath; don’t pull back the foreskin of a baby or young boy because it could be painful and cause harm
- Use a mild or non-perfumed soap (if you choose to use soap) to reduce the risk of skin irritation
- Avoid using talc and deodorants on your penis as they may cause irritation
- Circumcised men should also regularly clean their penis with warm water and a mild soap (if you choose to use soap).
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.







am diabetic can this problem be treated and what medication can help
Please consult a doctor for better diagnosis and treatment.
I am also suffering from this disease since many years, so I need advice how to overcome from it
Consult a doctor to undergo surgery option.
even me um suffering with that disease which medication can I use to treat it
Most probably surgery may recommed to cure this problem. So consult a doctor before taking medicines.
What are the steroid cream. Please give some best creams name and how to apply it.
Please consult a doctor to get creams and medicines for phimosis.