What is Phlebitis?
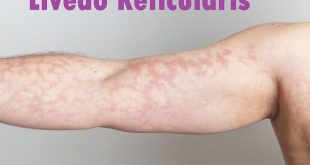
Phlebitis, also known as vein inflammation, is a medical condition characterized by the inflammation of a superficial vein, typically close to the surface of the skin. This inflammation occurs when a blood clot forms within the affected vein, leading to swelling, pain, and redness in the area. Phlebitis most commonly occurs in the legs, particularly in the veins just beneath the skin’s surface. While it can occur spontaneously, it is often associated with conditions that increase the risk of blood clot formation, such as prolonged inactivity, injury to the vein, or certain medical procedures.
Phlebitis in lower leg
The symptoms of phlebitis often include pain or tenderness along the course of the affected vein, swelling, warmth, and redness in the affected area. The condition can range from mild discomfort to more severe pain, depending on the extent of inflammation and clot formation. In some cases, phlebitis can be associated with a condition called deep vein thrombosis (DVT), where blood clots form in the deeper veins of the body, potentially leading to more serious health complications. It’s important to monitor and address symptoms of phlebitis promptly to prevent the progression of the condition and minimize the risk of complications.
Types of Phlebitis
It is characterized by the location of the affected veins:
- Superficial Phlebitis – Inflammation of veins near the surface of the skin is a less serious condition.
- Deep Vein Thrombosis – When phlebitis is in deeper veins, it is also known as Deep Vein Thrombosis (DVT).
- Thrombophlebitis – When the inflammation causes blood clotting, it is known as thrombophlebitis.
As with superficial phlebitis, acute superficial thrombophlebitis occurs just under the surface of the skin and should be monitored by a trained vascular physician. If phlebitis escalates to DVT and a clot occurs deeper in the body, the clot can migrate to other parts of the body and cause an embolism. Phlebitis generally occurs in leg veins, but vein inflammation can also affect arm veins.
Epidemiology
The prevalence and epidemiology of phlebitis vary based on several factors, including the underlying risk factors and the population studied. Phlebitis is more commonly observed in adults, with the incidence increasing with age due to factors like reduced mobility and higher prevalence of chronic medical conditions. Additionally, individuals with certain medical conditions such as obesity, diabetes, and cardiovascular diseases are more susceptible to developing phlebitis. Hospitalized patients, especially those undergoing intravenous therapy or postoperative recovery, are also at an increased risk due to the use of catheters and immobility.
The prevalence of phlebitis can be influenced by lifestyle factors, such as physical inactivity, smoking, and obesity. Occupations that involve prolonged sitting or standing can contribute to venous stasis, increasing the risk of clot formation and subsequent phlebitis. However, the actual prevalence of phlebitis can be challenging to determine precisely, as milder cases might go unreported and undiagnosed. In clinical settings, the incidence of phlebitis associated with intravenous catheters and medical procedures is monitored closely to reduce complications. Overall, understanding the epidemiology of phlebitis aids in identifying at-risk populations and implementing preventive measures.
Pathophysiology of Phlebitis
The pathophysiology involves a sequence of events that lead to inflammation and clot formation within a superficial vein. The process often begins with damage to the inner lining of the vein, which can result from various factors such as trauma, irritation from catheters or IV lines, or the slowing of blood flow due to immobility. This damage triggers an inflammatory response, during which immune cells and proteins are recruited to the site of injury. As a result, the vein’s inner lining becomes more permeable, allowing immune cells to enter the vessel wall and promoting the aggregation of platelets.
Subsequently, the combination of inflammation and platelet aggregation can lead to the formation of a blood clot, also known as thrombosis. This clot can partially or completely block the vein, contributing to the characteristic symptoms of phlebitis such as pain, redness, and swelling. The inflammatory response intensifies as the clot develops, further contributing to the discomfort and visible signs associated with the condition.
In some cases, the clot within the superficial vein may remain localized and resolve over time as the body’s natural anticoagulation mechanisms break it down. However, there is also a risk that the clot could extend into deeper veins, potentially leading to a more serious condition called deep vein thrombosis (DVT), where the clot forms in veins deeper within the body. Understanding the underlying pathophysiology of phlebitis is crucial for effective management and prevention of complications.
Symptoms of Phlebitis
The symptoms can vary in intensity and presentation, but they typically include:
- Pain or Tenderness: Pain and tenderness along the course of the affected vein are common symptoms of phlebitis. The pain can range from mild discomfort to more severe, throbbing pain, especially when pressure is applied to the area.
- Redness and Warmth: The skin over the inflamed vein often becomes red and may feel warm to the touch. This is due to the inflammatory response occurring in the vein and surrounding tissues.
- Swelling: Swelling in the area around the affected vein is a common symptom. This swelling occurs as a result of the inflammation and the buildup of fluids in the tissues.
- Hardening of the Vein: The affected vein might feel harder than usual due to the presence of the blood clot and the inflammation. This hardening can often be felt beneath the skin.
- Visible Red Lines: In some cases, you might see visible red lines along the path of the affected vein, indicating the inflamed area. These red lines can be a visual indication of the inflamed blood vessel.
- Skin Discoloration: Over time, the skin above the inflamed vein might darken or become discolored. This is a result of the inflammatory process and the increased blood flow to the area.
- Itching or Burning Sensation: Some individuals with phlebitis might experience itching or a burning sensation in the affected area. This discomfort can be due to the inflammation and irritation of the surrounding tissues.
It’s important to note that while phlebitis can occur on its own, it can also be associated with more serious conditions like deep vein thrombosis (DVT). Therefore, if you experience symptoms of phlebitis, especially if they are severe or accompanied by other concerning symptoms, it’s advisable to seek medical attention for proper diagnosis and treatment.
Causes of Phlebitis
Phlebitis has many causes, such as the following:
- Local trauma or injury to the vein
- Prolonged inactivity, such as long driving or plane rides
- Insertion of intravenous catheters (IV) in hospitals, or IV-induced phlebitis
- The period after surgery (post-operative period), especially orthopedic procedures
- Prolonged immobility, as in hospitalized or bed-ridden patients
- Varicose veins
- Underlying cancers or clotting disorders
- Disruption of normal venous system drainage because of removal of lymph nodes, for example, after mastectomy for breast cancer
- Intravenous drug use
- Patients with burns
Risk factors of Phlebitis
Some common risk factors include:
- Sedentary behavior for extended periods (for example, a long plane ride or car ride), obesity, smoking
- Estrogen-containing medications (including oral contraceptives and hormone replacement therapy
- Clotting disorders (which may predispose to easy clotting)
- Externally visible varicose veins
- Trauma to a varicose vein (for example, if your leg knocks into the dishwasher)
- Cancer
Another possible risk factor is venous reflux or venous insufficiency.
What are the complications of phlebitis?
Complications from superficial thrombophlebitis are rare. However, if you develop DVT, the risk of serious complications increases. Complications might include:
- Blood clot in the lungs (pulmonary embolism). If part of a deep vein clot becomes dislodged, it can travel to your lungs, where it can block an artery (embolism) and become potentially life-threatening.
- Lasting leg pain and swelling (post-phlebetic syndrome). This condition, also known as post-thrombotic syndrome, can develop months or years after you’ve had DVT. The pain can be disabling.
- Pulmonary embolism. A pulmonary embolism (PE) occurs when a blood clot gets stuck in an artery in the lung, blocking blood flow to part of the lung. Blood clots most often start in the legs and travel up through the right side of the heart and into the lungs. This is called deep vein thrombosis (DVT).
Diagnosis
Diagnosing phlebitis typically involves a combination of clinical assessment and, in some cases, imaging tests. Here are the steps involved in the diagnosis:
- Physical Examination: A doctor will examine the affected area, looking for signs of redness, warmth, swelling, and tenderness along the path of the vein. The appearance and location of these symptoms can provide important clues.
- Medical History: Your doctor will ask about your medical history, including any recent surgeries, injuries, or medical procedures, as well as any risk factors you might have, such as obesity, smoking, or a history of blood clotting disorders.
- Ultrasound: In some cases, an ultrasound may be used to visualize the affected vein and assess the presence of a blood clot. This non-invasive imaging technique can help confirm the diagnosis and determine the extent of the clot.
- Blood Tests: Blood tests are not usually necessary for diagnosing phlebitis, but they might be used to rule out other conditions or to check for clotting disorders in individuals with recurring cases.
- Differential Diagnosis: Sometimes, other conditions like cellulitis (skin infection), DVT, or varicose veins can present with similar symptoms. The doctor will consider these possibilities and rule them out if necessary.
It’s important to consult a healthcare professional if you suspect you have phlebitis or if you’re experiencing symptoms like pain, redness, and swelling in a vein. A proper diagnosis can help ensure appropriate treatment and prevent potential complications.
Treatment for Phlebitis
As painful and distressing as phlebitis can sometimes be, most cases are not serious and will resolve on their own over time.
Uncomplicated cases will typically respond to the following treatments aimed at easing pain and reducing local inflammation:
- Heat applications: Applying a heating pad or a hot water bottle to the affected area increases blood circulation and promotes healing.
- Elevating the leg: Propping up your feet as much as possible reduces blood pressure around the affected vein, easing pain and swelling.
- Compression stockings: Elastic compression socks, available over the counter or by prescription, prevent blood pooling in the lower limbs, reducing pain and swelling.
- Oral painkillers: Over-the-counter (OTC) nonsteroidal anti-inflammatory drugs (NSAIDs) like Advil (ibuprofen) and Aleve (naproxen) can also reduce inflammation and pain.
Additional treatments may be prescribed based on the severity of your symptoms and/or the location of the venous blockage, including:
- Anticoagulants: Also known as blood thinners, these may be used in people with varicose veins or those without varicose veins who have SVT in their thighs. Options include Arixtra (fondaparinux) and Lovenox (enoxaparin).
- Antibiotics: These prescription drugs may be used if there are signs of bacterial infection, such as fever and a pus-like discharge at the PIVC placement site.
- Hirudoid (heparinoid) cream: This prescription topical cream is commonly used to treat severe bruises caused by ruptured veins (known as hematomas).
- Surgery: Venous ligation and stripping is a surgical procedure in which the affected vein is tied off and removed through a small incision. It is commonly used to treat varicose veins.
Prevention
You can take control of actively preventing vein inflammation and other venous conditions yourself by minimising the influenceable risk factors that have been described. Some tips:
- Basic therapy: Wear medical compression stockings on a daily basis if your legs are prone to varicose veins.
- Exercise: Avoid long periods of standing and sitting, and do vein exercises to activate your venous pump
- Sport: Activities such as swimming, hiking and Nordic walking activate your veins.
- Drink plenty of water: A lack of fluids makes the blood thicker, meaning that your risk of blood clots increases.
- Go to your doctor: Have your varicose veins treated.
- Risk factor: Take care of your health: Give up smoking because smoking alters the vascular walls.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.