What is Uterus Didelphys?
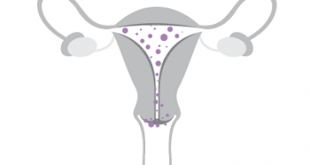
Uterus didelphys, also known as double uterus, is a rare congenital condition in which a woman is born with two separate uteri, each with its own cervix and in some cases, a double vagina. This condition occurs during fetal development when the Müllerian ducts, which eventually form the uterus, fail to fuse properly, leading to the formation of two distinct uteri instead of one. Women with uterus didelphys often have normal external genitalia, making it difficult to diagnose the condition without medical imaging.
Having a double uterus does not typically cause symptoms, and many women with this condition may not even be aware of it until they undergo a medical examination for unrelated issues, such as infertility or recurrent miscarriages. However, uterus didelphys can sometimes lead to complications during pregnancy, such as a higher risk of miscarriage, preterm birth, or breech presentation. In some cases, surgical intervention may be necessary if there are complications or if a woman with uterus didelphys wishes to conceive and carry a pregnancy to term. Overall, while uterus didelphys is a rare condition, with proper medical care and monitoring, women with this condition can lead healthy lives and have successful pregnancies.
x
Types of Uterus Didelphys
Uterus didelphys is a broad term that encompasses several variations of the condition, including:
Uterus Didelphys (Class I)
In this type, there are two separate uteri, each with its own cervix. Additionally, each uterus has its own vaginal canal. Women with this type have a complete double reproductive system, including two uteri, two cervixes, and two vaginas.
Uterus Didelphys with Blind Hemivagina (Class II)
In this variation, a woman has two uteri, two cervixes, and two vaginas, but she also has a septum (wall) in her vaginal canal, which creates a blind hemivagina on one side. This septum can cause menstrual blood to accumulate in the affected hemivagina, leading to pain and discomfort. Surgical intervention may be required to correct this condition and alleviate symptoms.
Uterus Didelphys with Hematocolpos (Class III)
This type involves having two uteri, two cervixes, and a single vagina. However, there is a septum in the vaginal canal, causing the accumulation of menstrual blood in the vagina (hematocolpos). This condition can lead to cyclic pelvic pain and may require surgical intervention to remove the septum and alleviate symptoms.
Uterus Didelphys with Hematometrocolpos (Class IV)
This is the most complex form of uterus didelphys. It involves having two uteri, two cervixes, a single vagina, and a septum in the vaginal canal. Additionally, there is a septum within each uterus, creating a double-chambered structure. Menstrual blood accumulates in both uteri and the vagina, leading to significant discomfort. Surgical correction is often necessary to remove the septa and alleviate symptoms.
It’s important to note that the specific type and severity of uterus didelphys can vary among individuals, and the appropriate treatment depends on the individual’s symptoms and reproductive goals.
Epidemiology
Uterus didelphys is a rare congenital anomaly of the female reproductive tract, with an estimated prevalence of approximately 0.1% in the general population. This means that about 1 in 1,000 women might be affected by this condition. Uterus didelphys occurs sporadically, and while its exact cause remains unclear, it is believed to result from a complex interplay of genetic and environmental factors during embryonic development. This condition is often diagnosed during adolescence or early adulthood when a girl or woman experiences abnormal menstrual bleeding or pelvic pain. Despite its rarity, uterus didelphys has significant clinical implications, especially in the context of reproductive health. Early detection and proper management are crucial for addressing potential complications during pregnancy and ensuring optimal maternal and fetal outcomes. Research into the epidemiology of uterus didelphys continues to shed light on its prevalence and associated factors, aiding healthcare professionals in better understanding and addressing this rare condition.
Pathophysiology of Uterus Didelphys
Uterus didelphys is a congenital uterine malformation that arises during fetal development. During normal embryonic growth, two separate ducts known as Müllerian ducts fuse together to form a single uterus. In the case of uterus didelphys, this fusion process is either incomplete or does not occur at all. This results in the development of two separate uteri, each with its own cervix, and sometimes accompanied by a double vagina. The exact cause of this condition remains largely unknown, although genetic and environmental factors are believed to play a role. Mutations in certain genes or disruptions in the signalling pathways responsible for Müllerian duct development could potentially lead to this anomaly. Additionally, hormonal imbalances or exposure to certain teratogenic agents during early pregnancy might contribute to the abnormal development of the uterus.
From a physiological standpoint, women with uterus didelphys often have normal reproductive functions, including regular menstrual cycles and the ability to conceive. However, the condition can pose challenges during pregnancy. The presence of two separate uteri increases the risk of complications such as preterm labour, breech presentation, and caesarean section deliveries. Additionally, women with this condition may have a higher likelihood of miscarriages or pregnancy loss, although many are able to carry pregnancies to full term successfully. Understanding the pathophysiology of uterus didelphys is essential for healthcare providers to anticipate and manage potential complications effectively, ensuring the best possible outcomes for both the mother and the baby.
What are the symptoms of uterus didelphys?
For some, this irregularity is detected during a routine check-up or when other symptoms appear. Some of these symptoms include:
- Uncontrollable bleeding when using a tampon
- Heavy bleeding during a period
- Unusual cramping before or after menstruation
- Repeated pregnancy loss
- Preterm labour
- Painful sexual intercourse
During a check, the doctor may order imaging tests, such as magnetic resonance imaging (MRI), to determine the diagnosis. Depending on the severity and nature of the condition, a treatment may then be proposed. Some women with uterus didelphys require no treatments and may even carry on with their pregnancies successfully.
Causes of Uterus Didelphys
Although the exact cause for this condition is unknown, experts have been researching this topic, and below we are bringing you some of the most common reasons why certain other developments in the body can affect the development of uterine didelphys.
- Certain previous genetic conditions
- Herlyn-Werner-Wunderlich syndrome, where there are rare Mullerian duct abnormalities that can cause the blockage of one part of the double vagina
- Small kidneys or only one kidney
- Being born without a cervix, i.e., cervical agenesis
- A condition that causes the leakage of urine called congenital vesicovaginal fistula
- The bladder growing outside of the body in the uterus
- Being born without a vagina, i.e., vaginal agenesis
These are certain conditions that can significantly impact the development of a double uterus condition, but as said, it is still to be determined what the exact cause of this issue is.
What are the risks of uterus didelphys pregnancy?
Pregnancy in women with uterus didelphys comes with certain risks that need to be carefully managed. Here are five potential risks associated with such a pregnancy:
- Miscarriage
Women with uterus didelphys have an increased risk of miscarriage, particularly during the first trimester. The abnormalities in the uterine structure can make it challenging for a pregnancy to implant and develop properly.
- Preterm birth
Uterus didelphys is associated with a higher risk of preterm delivery. The unique structure of the double uterus can cause mechanical issues that may lead to premature labor.
- Malpresentation
Babies born to women with uterus didelphys may have a higher chance of being in a breech or transverse position. This can increase the likelihood of complications during delivery and may necessitate a cesarean section.
- Placental abnormalities
Uterus didelphys can increase the risk of placental abnormalities, such as placenta previa or placenta accreta. These conditions can have serious implications for both the mother and the baby.
- Uterine rupture
In rare cases, the presence of a double uterus can increase the risk of uterine rupture during labor. This is a life-threatening emergency that requires immediate medical intervention.
Are there health risks associated with uterus didelphys?
Most people who have a double uterus lead healthy lives and don’t have any significant health complications. The following risks are associated with a double uterus:
- Complications during pregnancy including miscarriage and premature birth.
- Increased risk for cesarean section due to because your baby isn’t well positioned for birth.
- Heavy menstrual bleeding.
- Mispositioned or missing kidney.
Complications of Uterus Didelphys
Women with a double uterus can usually get pregnant. It’s possible to carry your baby to full term, but with uterine didelphys, you have a greater risk of pregnancy complications.
These complications can include:
- Repeated pregnancy loss
- Early labor
- Torn vaginal tissue between the two vaginas during labor
- Breech baby (facing feet first) who needs a C-section delivery
- Low birth weight
- Intrauterine growth restriction
- Kidney problems
Some doctors disagree about whether women who have uterine didelphys should have a vaginal delivery or a C-section. The researchers of one review show that vaginal delivery is possible but feel that a C-section might be the safest.
Uterine didelphys is also linked with some other conditions like endometriosis. This condition happens when tissue similar to the uterus lining tissue called endometrium grows outside of the uterus but still responds to hormones. This tissue breaks down and bleeds as normal but has no escape, which causes lots of pain.
Diagnosis
A regular pelvic examination could indicate a second uterus. A double cervix or a uterus with an unusual shape may be felt by your doctor. You might require particular testing to confirm the diagnosis of a double uterus:
- Ultrasound: Images of the inside of your body are produced during this test using high-frequency sound waves. During the procedure, a transducer is placed on the exterior of the lower abdomen to record the images. The transducer could also be inserted into your vagina. It is known as Transvaginal ultrasonography. The optimum view might require using both kinds of ultrasonography.
- Sonohysterogram: Sonohysterograms are a specific type of ultrasound examination. Through a tube, fluid is pumped into your uterus. On the ultrasound scan, the fluid can be seen to outline your uterus’ shape. This enables your doctor to check for any unexpected symptoms.
- (MRI) Magnetic resonance imaging: The MRI scanner resembles a tunnel with open ends. On a portable table that slides into the tunnel’s entrance, you lie down. A magnetic field and radio waves are used in this painless test to produce cross-sectional images of the interior of your body.
- Hysterosalpingography: Through your cervix, a specific dye is injected during a hysterosalpingography procedure into your uterus. X-rays are obtained when a dye is injected into your reproductive system. These photos demonstrate your uterus’s size and form. Additionally, they reveal whether your fallopian tubes are open.
- Additionally, an MRI or ultrasound may be used to look for renal issues.
Treatment
The treatment for uterus didelphys depends on the specific symptoms and complications experienced by the individual. Here are some common treatment approaches:
Management of Symptoms
If a woman with uterus didelphys does not experience significant symptoms or complications, she may not require any treatment. Regular gynaecological examinations and monitoring can ensure her reproductive health is maintained.
Surgical Interventions
Surgical treatment may be necessary in cases where there are complications such as:
- Septum Resection: For individuals with a septum in the uterus or vagina, a surgical procedure called septum resection or metroplasty can be performed. This surgery involves removing the septum, allowing for a more normal uterine or vaginal structure. This can improve symptoms and increase the chances of successful pregnancy.
- Hematocolpos or Hematometrocolpos Drainage: In cases where menstrual blood accumulates in the vagina or uteri due to obstructed menstrual flow, the accumulated blood may need to be drained. This can be done through a minor surgical procedure to alleviate pain and discomfort.
Fertility Treatments
Some women with uterus didelphys can conceive naturally and have successful pregnancies. However, fertility treatments such as in vitro fertilization (IVF) may be recommended in cases where there are difficulties conceiving due to the anatomical abnormalities.
Management of Pregnancy
If a woman with uterus didelphys becomes pregnant, close monitoring by healthcare professionals is essential. Complications such as miscarriage, preterm birth, or breech presentation are more common, so appropriate medical care and surveillance during pregnancy are crucial to ensure a healthy pregnancy and delivery.
Psychological Support
Coping with a congenital condition such as uterus didelphys can be emotionally challenging. Psychological support and counselling can be beneficial for individuals and couples dealing with the condition, especially if it affects their reproductive goals and experiences.
How to prevent uterus didelphys?
While the exact cause of this condition is unknown, there are no specific ways to prevent it. Uterus didelphys is a result of abnormal development in the fetal stage, and it is not caused by any actions or behaviours during pregnancy or otherwise.
However, it’s important for women to maintain overall good health before and during pregnancy to minimize the risk of complications during pregnancy and childbirth. Here are some general health tips that can help in promoting a healthy pregnancy and reduce the risk of complications:
- Regular Health Checkups: Regular visits to the gynaecologist can help in early detection and management of any reproductive health issues.
- Healthy Lifestyle: Maintaining a balanced diet, exercising regularly, and avoiding harmful substances such as tobacco, alcohol, and illicit drugs can contribute to overall reproductive health.
- Preconception Planning: If you are planning to conceive, it’s important to discuss your medical history and any concerns with a healthcare provider before getting pregnant.
- Manage Chronic Conditions: If you have any chronic conditions like diabetes or hypertension, managing them effectively can reduce the risk of complications during pregnancy.
- Genetic Counselling: If there is a family history of congenital conditions, genetic counselling can provide information and support for making informed decisions about family planning.
- Prenatal Care: Early and consistent prenatal care is essential for monitoring the health of both the mother and the developing fetus.
- Avoid Infections: Preventing infections, especially during pregnancy, is crucial. Practicing good hygiene and avoiding contact with individuals who are sick can help in reducing the risk of infections.
- Emotional Well-being: Managing stress and seeking emotional support can contribute to a healthy pregnancy. Stress reduction techniques such as yoga, meditation, or counseling can be beneficial.
Remember, while these tips promote overall reproductive health and a healthy pregnancy, they cannot specifically prevent the occurrence of uterus didelphys, which is a rare congenital condition.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.