Eosinophilia – Definition, Causes, and Treatment.
Definition
Eosinophilia indicates elevated levels of eosinophils in the peripheral blood, usually related to an infectious, neoplastic, or allergic process. Often, high numbers of eosinophils may be present in other body fluids or tissues, but the term typically refers to peripheral blood eosinophilia. It is often defined as an absolute eosinophil count of ≥500 eosinophils/microliter (cells/microL) of blood. 500-1500cell/microL is considered mild, 1500-5000 cells moderate, and >5000 severe.
Pathophysiology
Allergic reactions are associated with a raised eosinophil count, slight at first but increasing with each exposure. Mast cells and basophils associated with a hypersensitivity reaction produce and release a number of cytokines, which evoke IgE production. IgE, elevated levels, stimulates eosinophil production. IL-5 is a chemokine that is extremely important in the final differentiation of mature eosinophils, as well as their recruitment into sites of inflammation, and their prolonged survival.
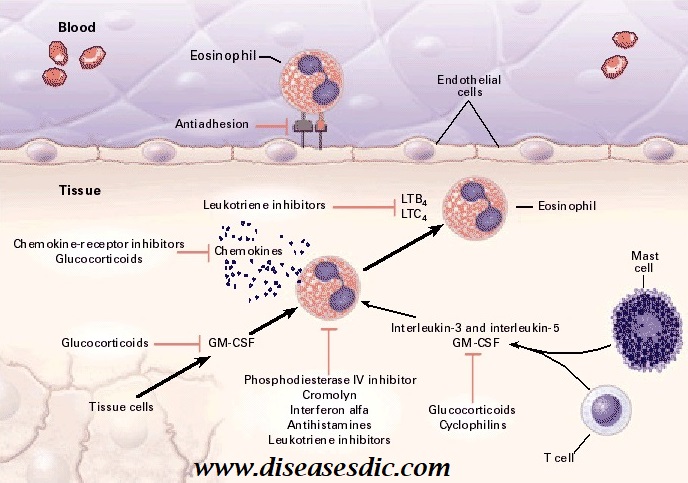
In addition, eosinophils produce growth factors which are responsible for the fibrotic response to inflammatory injury in affected tissues. This is because the eosinophils release cytokines which not only induce
Types
Eosinophilia is classified as primary or secondary, in addition to the hypereosinophilic syndromes.
Primary Eosinophilia
- Primary eosinophilia is a rise in the peripheral eosinophil count without any underlying condition to account for it. It is subclassified into clonal and idiopathic types.
- Clonalprimary eosinophilia is the type of eosinophilia that is due to the proliferation of a clone of eosinophils in the bone marrow and is found in leukemias or other myeloproliferative disorders. Idiopathic primary eosinophilia is a term used to refer to peripheral blood eosinophilia without any detectable cause.
Secondary Eosinophilia
Secondary eosinophilia is the result of other disorders not associated with bone marrow proliferation, such as atopy, asthma, and most commonly helminthic infestations.
Hypereosinophilic Syndromes
Hypereosinophilic syndromes are disorders which are characterized by eosinophilia above 1500/µL persisting for at least 6 months, with no underlying disease
- Churg-Strauss syndrome
- Tropical pulmonary eosinophilia
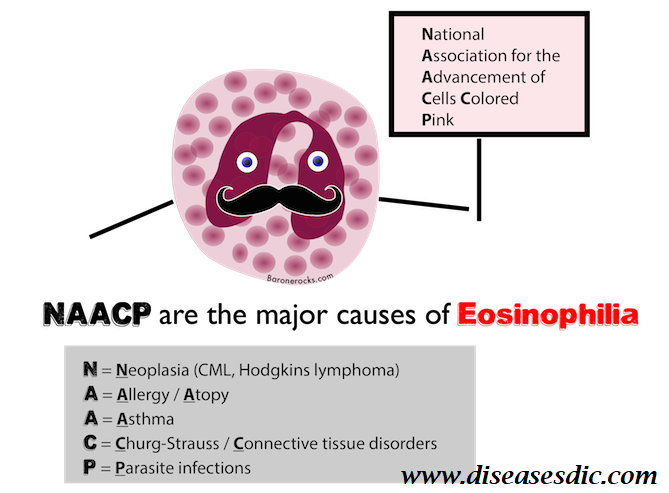
Causes and Risk factors
There are numerous reasons your eosinophil count may be elevated. Some of the causes are benign and require little treatment. It is not uncommon for the elevated count to be transient and resolve without treatment. Let’s review some of the causes now.
Parasite infections: The most common cause of eosinophilia is a parasite infection include schistosomiasis, trichinosis, strongyloidiasis, and ascariasis.
Drug reactions: Medications can trigger eosinophilia, sometimes without any obvious signs or symptoms. The most common medications associated with eosinophilia include antibiotics (penicillin, cephalosporins), non-steroidal anti-inflammatory medications (aspirin, ibuprofen), ranitidine (for gastroesophageal reflux), phenytoin (anti-seizure) and allopurinol (used to treat gout). The most severe form is called drug reaction with eosinophilia and systemic symptoms (DRESS). Fortunately, most people will not have these reactions when they receive these medications.
Atopy: Atopy is a particular reaction that occurs in the body. Typically, atopy refers to asthma, seasonal allergies (also called allergic rhinitis), and eczema. It is not uncommon for someone to have more than one of these medical conditions as they are related. These are some of the most common causes of mild to moderate eosinophilia, particularly in children. Similarly, food allergies can also cause elevated eosinophil counts.
Eosinophilia esophagitis (EoE): This is a disorder characterized by eosinophils spreading to esophagus which normally does not contain eosinophils. About 50% of people with EoE will also have elevated eosinophil counts in the blood.
Cancers: There are several cancers, particularly blood cancers that are known for increasing the eosinophil count. These include a rare type of acute myeloid leukemia (AML) called eosinophilic leukemia. Other causes include several of the myeloproliferative neoplasms (such as, essential thrombocythemia, polycythemia vera) B-cell and T-cell lymphoma, as well as adenocarcinomas of the gastrointestinal tract, lung, and cervix.
Clinical Manifestations
Symptoms of eosinophilia vary based on the underlying conditions.
- Frequent wheezing and breathlessness are symptoms typical to eosinophilia caused due to asthma.
In case of eosinophilia due to parasitic infections symptoms may include
- Abdominal pain
- Diarrhea
- Fever
- Cough
- Rashes
- Frequent infections
- Abscesses
- Pneumonia
- Mouth sores
Few other symptoms of eosinophilia include
- Weight loss
- Night sweats
- Enlargement of lymph nodes
- Skin rashes
- Tingling and numbness due to nerve damage, these symptoms however occur rarely.
Complications arises during Eosinophilia
- Weight loss
- Night sweats
- Lymph node enlargement
- Skin rashes
- Numbness and tingling due to nerve damage
- Wheezing
- Breathlessness
In case of eosinophilia types following complications arise
- Myocardial fibrosis
- Chronic heart failure
- Death
Diagnosis and Test
History
First, a careful history is taken, to elicit travel to places where helminthiasis is rife; exposure to drugs; ingestion of possibly helminth-infected food; family history of myeloproliferative disorders, allergies, and drug hypersensitivity.
Symptoms which should be inquired about include:
- Those of helminth infestation
- Symptoms of organ involvement such as lung infiltration, inflammatory bowel disease, or vasculitis of various organs
- Symptoms of allergies of the skin or respiratory system in particular
- Systemic symptoms such as fever, joint pain
and swelling, or lymphadenopathy
Drug exposure should be classified based on the association between the drug and the chances of eosinophilia. For instance, anticonvulsants, allopurinol (a drug used in gout), and semisynthetic penicillins have a higher chance of causing eosinophilia.
Specific findings may also point to the culprit drug, such as:
- Anticonvulsants, if hepatitis or DRESS is present
- NSAIDs or semisynthetic penicillins in pneumonitis
- Immunevasculitis with phenytoin or allopurinol
- Nephritis with cephalosporins
Physical Examination
The patient should have a detailed examination of the cardiovascular, renal, respiratory, gastrointestinal, and neurologic systems. Such findings as a skin rash, asthma or lung congestion, or generalized lymphadenopathy are suspicious of underlying conditions such as pulmonary syndromes with eosinophilia, myeloproliferative disorders, and vasculitis or atopic disease. This examination will also help to pick up complications due to hypereosinophilia, the most important of which include pulmonary, neurologic, and cardiac dysfunction.
Screening and Testing
In addition to the basic blood counts which revealed the eosinophilia, other tests may include:
- Peripheral blood smear for abnormal eosinophils or blast cells suggestive of myeloproliferative disorders
- Stool ova and parasite tests on three consecutive specimens
- Parasite tests such as thin and thick blood smears
- Specific serological tests for parasites
- Anti-neutrophil cytoplasmic antibodies which are raised in some types of immune disease
- Organ-specific tests such as renal or hepatic function tests as clinically indicated
- Chest radiograph
- Electrocardiogram,cardiac troponin
- IgE levels and other immunoglobulins
- Urinalysis
- Serologic tests for vasculitis and other connective tissue disorders
- Specialized tests such as bone marrow aspirate examination and cytogenetic tests for myeloproliferative disorders
- Echocardiography if other tests are normal, or if cardiac symptoms are present
- Pulmonary function tests
- Tissue biopsies for parasites such as Trichinella, filariasis, and visceral larva
migrans - Imaging tests based on symptoms or signs of organ involvement, such as CT scan of the chest or abdomen
Treatment and Medications
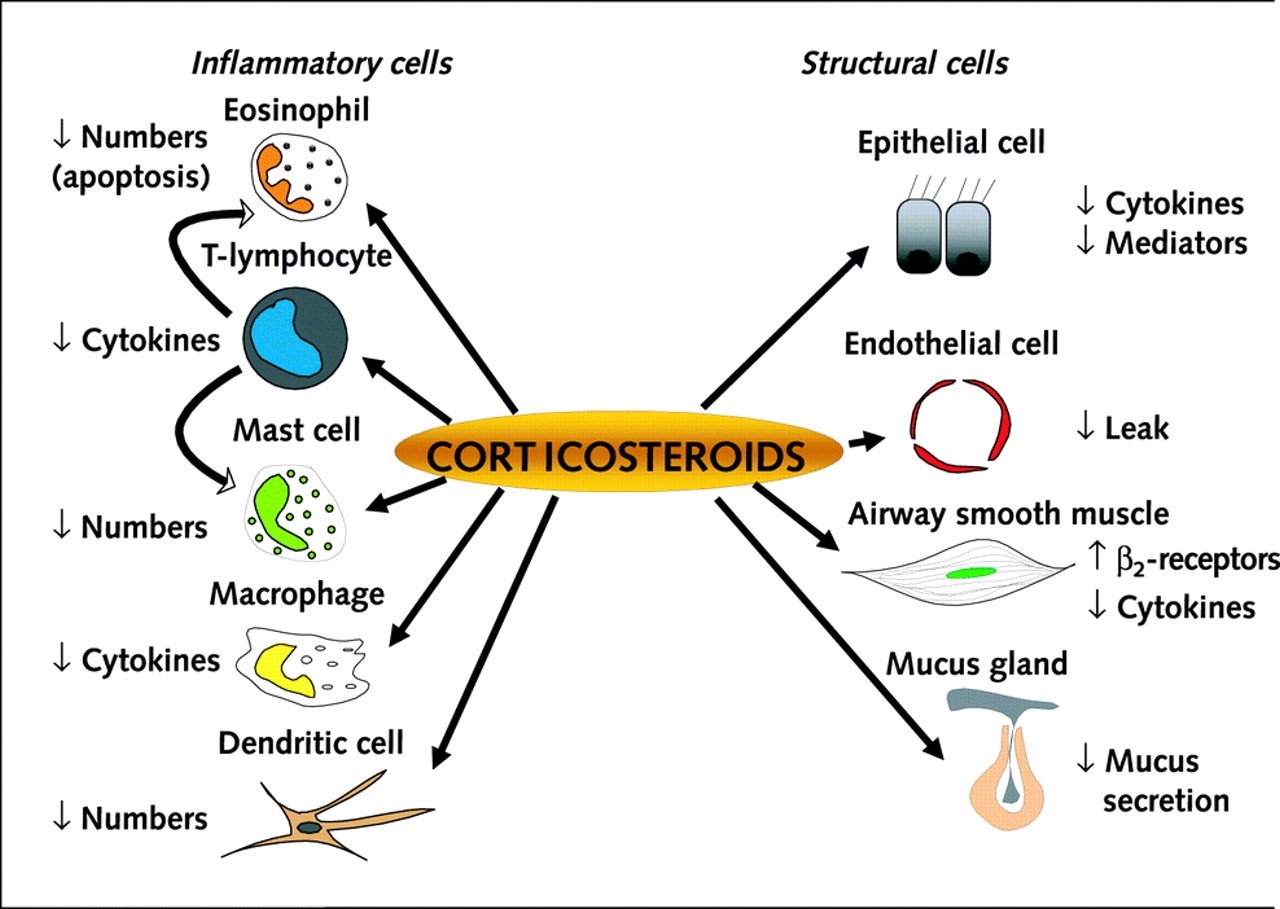
Treatment tackles the underlying cause of the condition, whether it is caused due to allergens, medical reaction or a parasitic reaction. Treatments such as intake of oral Corticosteroid drugs which are steroid hormones produced from the adrenal cortex of the vertebrates. Corticosteroid drugs such as Prednisolone are preferred at single doses of 30–60mg. These treatments are effective and non-toxic.
Natural Home Remedies foreosinophilia
- Ginger, it is a very good herb in lowering down the increase count of eosinophils. It is taken by preparing its juice by mashing it properly and put this in a tea drink this tea one to two times daily for
few days which gives better results. - Turmeric powder is a very good remedy to treat patients who have higher values of eosinophils. It is prepared by putting a pinch of turmeric powder in one glass of water and makes it boil and drink.
- Ginseng is a very good home remedy in reducing the inflammation in airways and thus lowers down the count of high eosinophils.
- Eucalyptus its oil is used in reducing the various symptoms in eosinophilia.
- Fenugreekits seeds are used in combating the infections that are related to increasing eosinophilia. The seeds of fenugreek are boiled in one glass of water the two tablespoons of seeds are added in a glass of water drink this mixture every day morning and evening.
- HolyBasil (Tulsi leaves) it is a very effective home remedy known for treating high eosinophilic count. The chewing of two to three leaves is recommended for better results.
- Malabar Nut It is the very useful home remedy in reducing the symptoms of eosinophilia. Drink its juice daily for better results.
- Neem(Azadirachta indica) It is used as medicine since many years it has a property of anti-bacterial, antifungal, antiviral, sedative, anti-diabetic so it is useful for various purposes it helps in removing unwanted harmful toxins from the body. Thus it is helpful in controlling various types of allergies related to food, in the
skin like eczema, psoriasis etc.
Prevention of Eosinophilia
Cause of eosinophilia is not always clear. As a result, there are no specific steps to prevent eosinophilia.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.




is bronchitis and cough caused due to esonofolia is curable by Ginger?
I get frequent Cough due to increased esonofolia. and Ginger does help. What numerical count while blood test is considered within limits
Generally, eosinophilia is an incurable disease the treatments are used to ease the pain caused by it.
an increase in the number of eosinophils in the blood, occurring in response to some allergens, drugs, and parasites, and in some types of leukaemia.homeopathy is the best treatment for Eosinophilia it cures completely with out any side effects.for more info:Homeopathy Treatment for Eosinophilia
Nice artlcle on eosinophilia.
congrats
Very nice words used in article on allergies or eosinophils and easy to understand the matter and very very beneficial for all, who suffering by such type of diseases.
Since a child I have bronch athma acute athma heritage from my father and lack of immunity what is treatment for lack of immunite
There are two main types of medications used to treat asthma:
Long-term control medications such as inhaled corticosteroids are the most important medications used to keep asthma under control. …
Quick-relief inhalers contain a fast-acting medication such as albuterol.