Definition
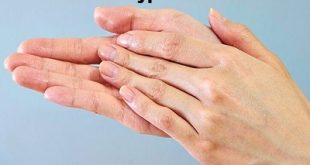
Burning feet syndrome, also referred to Grierson-Gopalan syndrome, causes severe burning and aching of the feet, and changes of the feet that lead to excessive sweating. This medical condition can even affect the eyes. The condition occurs more frequently in women and is often a problem when a person is between 20 and 40 years old.
This can occur due to Hereditary factors or Mechanical factors such as mechanical compression of the peripheral nerves (as seen in tarsal tunnel syndrome) and in diseases such as hypothyroidism, diabetes, and rheumatoid arthritis.
Studies have also related this condition to
- Psychosomatic causes
- Vitamin B deficiency
- Renal failure (dialysis patients)
- Hypothyroidism
Nerve entrapment can occur at the level of the tarsal tunnel adjacent to the medial malleolus. Nerve entrapment due to sciatic mononeuropathy and spinal arteriovenous malformation can also cause burning feet. Burning is usually limited to the soles of the feet but may ascend to involve the top of the ankles or lower legs. The arms and palms of the hands are spared. A few patients occasionally complain of pins and needles or tingling in the lower extremities. Symptoms show worsening at night with day time improvement. Patients with underlying psychiatric disorders may present with a myriad of psychosomatic.
Signs and symptoms in association with burning feet. On examination, there is a paucity of objective signs. The overlying skin and blood vessels are normal in most, while in some patients there may be accompanying erythema of the feet with warm overlying skin as in erythromelalgia. There is no local tenderness over the affected parts. If the condition is being caused by a disease i.e. Diabetes, Hyperthyroidism, Psychosomatic, etc than disease-specific measures must be taken.
Causes of Burning Feet Syndrome
While fatigue or skin infection can cause temporary burning or inflamed feet, burning feet are most often a sign of nerve damage (peripheral neuropathy). Nerve damage has many different causes, including diabetes, chronic alcohol use, exposure to certain toxins, certain B vitamin deficiencies, or HIV infection.
Possible causes of burning feet:
- Alcohol use disorder
- Athlete’s foot
- Charcot-Marie-Tooth disease (a group of hereditary disorders that affects the nerves in your arms and legs)
- Chemotherapy
- Chronic kidney disease
- Complex regional pain syndrome (chronic pain due to a dysfunctional nervous system)
- Diabetic neuropathy (nerve damage caused by diabetes)
- HIV/AIDS
- Hypothyroidism (underactive thyroid)
- Tarsal tunnel syndrome
- Vitamin deficiency anemia
Burning Feet Syndrome Symptoms
The most common symptoms of burning feet syndrome include:
- Sensations of heat or burning, often worsening at night
- Numbness in the feet or legs
- Sharp or stabbing pain
- Feeling of heaviness in the feet
- Dull ache in the feet
- Skin redness or excess warmth
- Prickling or tingling or a feeling of “pins and needles”
Complications
Because burning feet can be due to serious diseases, failure to seek treatment can result in serious complications and permanent damage. Once the underlying cause is diagnosed, it is important for you to follow the treatment plan that you and your health care professional design specifically for you to reduce the risk of potential complications including:
- Brain damage (if the sensation of feet burning is due to stroke)
- Loss of limb
- Permanent nerve damage
Diagnosis and test
Most people who have burning feet have a likely cause (such as diabetes) that can be identified. For these people, the diagnosis of burning feet due to neuropathy is straightforward, and additional testing is not needed. In a few people whose burning sensation is sudden, rapidly worsening, or has no explainable cause, further testing may be needed to make a correct diagnosis. These tests may include:
Electromyography (EMG): A test of muscle function using recordings of electrical activity inside the muscles. A probe may be placed on the skin, or a needle may be inserted into the muscle, for an EMG test.
Nerve conduction study: A nerve conduction study tests the ability of nerves to transmit impulses. A nerve is stimulated, and the response in the muscle controlled by that nerve is measured.
Laboratory tests: Sometimes, tests of blood, urine, or spinal fluid may be suggested to help diagnose the cause of burning feet. Vitamin levels can be checked with a simple blood test.
Nerve biopsy: Very rarely, a doctor may suggest cutting out a piece of nerve tissue and examining it under a microscope.
Treatment and medications
The main aim of treatment is to prevent any further damage to the nerves. In general, the treatment can be mainly classified as pharmacological and nonpharmacological. The treatment procedure depends on the cause of the problem and other co-morbidities of the patient.
Treating the underlying cause of the burning in the bottom of feet will help in the improvement of the symptoms, such as in the case of peripheral neuropathy caused by:
Diabetes mellitus – Proper dietary modifications with oral hypoglycemic drugs or insulin injections to maintain the blood glucose level within the desired range.
Alcoholism – Taking proper measures to stop further alcohol intake and medications to cure the alcohol withdrawal syndrome to prevent further nerve damage.
Vitamins and other nutritional deficiencies – Proper dietary supplements given orally or intramuscularly to maintain the required levels.
Chronic kidney disease – Hemodialysis or peritoneal dialysis to remove the excess toxins.
Hypothyroidism – Proper oral medications to bring the thyroid hormone levels back to normal.
HIV/AIDS – Proper treatment according to the condition of the patient.
Guillain-Barre Syndrome (GBS) and chronic inflammatory demyelinating polyneuropathy (CIDP) – plasmapheresis and immunoglobulin therapy.
If the symptoms are due to peripheral artery disease treatment should involve lifestyle modification such as exercises, quitting smoking, and a healthy diet in addition to lipid-lowering drugs to maintain proper lipid levels. Sometimes surgeries will be needed too.
Self-treatment of the burning foot sensation:
The most important part of managing burning feet yourself is to get it checked to make sure it is not caused by one of the rare serious problems.
Once the cause is established, there are a number of things that you can do to help your burning feet, but this can depend on the cause:
- If it’s mechanical, well-fitting shoes with support is a good place to start to help.
- If hot and sweaty, there are various self-treatments for the sweaty foot
- Creams or ointments with cooling properties can help relieve the symptoms
- Some relief in some people has been shown to occur with the use of magnets
- Wear socks made of cotton rather than synthetic fabrics
- Bath feet in cool water
- Avoid prolonged period of standing
- Cushioning or shock-absorbing insoles may make standing more tolerable
There is a lot of advice on the internet to take vitamin B12 to help burning feet. However, a burning foot occurring with the neuropathy that is associated with a deficiency of vitamin B12 is very uncommon and should be managed by a medical doctor. The taking of B12 for burning feet is not likely to help unless a deficiency is a cause and it is one of the more uncommon causes of the burning foot.
Some commonly prescribed medications for burning feet include:
- Gabapentin (Neurontin)
- Amitriptyline (Elavil)
- Desipramine (Norpramin)
- Carbamazepine (Tegretol)
- Pregabalin (Lyrica)
- Duloxetine (Cymbalta)
- Topiramate (Topamax)
- Venlafaxine (Effexor XR)
Other pain medications may be necessary to reduce the severe discomfort some people experience from burning feet. Over-the-counter medicines like Advil, Aleve, Motrin IB, and Tylenol control pain in many people with burning feet. Prescription pain relievers like tramadol (Ultram) or low-dose opiates (narcotics) may be necessary for severe pain.
Other treatment considerations include:
Use of creams that improve the blood flow to the joints and blood vessels of the foot. Certain creams and vitamin B supplements can also be helpful in reducing the burning sensation.
- Use of magnetic therapy insoles to assist in relieving the burning sensations.
- Reduction/elimination of alcohol consumption and smoking.
- Use of shoes and socks that have adequate ventilation and are comfortable. In cases where it is a mechanical failure, arch supports and wider shoes may relieve discomfort. If the underlying cause is flat feet, orthotics will help restore the foot arch. Wearing cotton socks is also recommended.
- Soaking the feet daily in cold water for 15 minutes. This can bring temporary symptomatic relief. You should avoid exposing your feet to the heat.
Prevention
There is no way to completely prevent burning feet, but these guidelines may help to address some problems.
- Schedule regular examinations with a podiatrist or foot care specialist: Regular checkups are necessary if you have diabetes or other conditions that can affect the nerves. People with diabetes or other conditions may need to be fitted with special shoes.
- Select shoes that fit properly and provide adequate ventilation: Shoes should have low heels, a wide toe box, and provide good support for the arches of the foot.
- Wear clean, dry socks to prevent athlete’s foot: Change your socks often if you participate in sports or other activities that cause the feet to perspire.
- Examine your feet daily for signs of infection or injury: Check your feet for blisters, sores, cuts, ulcers, and breaks in the skin to prevent infections.
- If you have diabetes, controlling your sugar may be the single most effective method of preventing or treating neuropathy secondary to this cause.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.