Definition
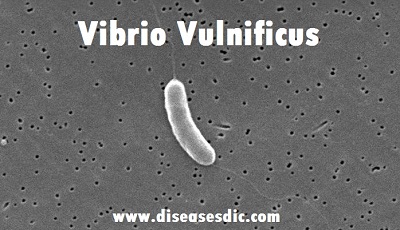
Vibrio vulnificus is a bacterium that occurs naturally in marine and estuarine waters throughout the world. It thrives in warm waters (especially warmer than 18ºC) and it is therefore common in tropical and subtropical estuarine and sea waters. The bacterium can be present in the water itself and in shellfish that grow in these waters.
For the majority of people, the bacterium is harmless. However, people who wade or swim in estuarine or sea water with wounds or breaks in their skin, or who ingest raw or undercooked shellfish, may be at risk of infection. Infections are uncommon and are usually mild. However, on rare occasions, Vibrio vulnificus may cause life-threatening infections.
People with chronic liver diseases including hepatitis, cirrhosis, haemochromatosis (iron storage disease), and liver cancer; and people with chronic diseases such as diabetes, chronic kidney disease, or conditions that impair the immune system, are at a higher risk of serious infection. People who take prescribed medication to decrease stomach acid levels or who have had gastric surgery are also at higher risk.
Epidemiology of Vibrio Vulnificus
This disease is not transmitted from person to person. Sporadic cases are reported each year. Vibrio vulnificus is a free-living organism found in marine waters. This organism is of special concern to the oyster industry and is found routinely in cultured oysters. This is a very serious disease in that approximately one-third of the patients seen for care associated with wound infections are either in shock or develop hypotension within 12 hours of hospitalization. Three-quarters of the patients develop bullous skin lesions, thrombocytopenia, and often disseminated intravascular coagulation.
Over 50% of the patients with primary septicemia die and the mortality rate exceeds 90% among those who become hypotensive. Vibrio vulnificus can also infect wounds sustained while in contact with coastal or estuarine waters (boating accidents, fisherman oyster shuckers) and can range from mild, self-limited lesions to rapidly progressive cellulites and myositis.
Pathophysiology
The morphology of Vibrionaceae contributes significantly to its virulence. Structurally V. vulnificus is a flagellated motile halophilic bacillus with a capsular polysaccharide (CPS), a lipopolysaccharide (LPS), and specific flagellin homologous proteins (FHPs).
Capsular polysaccharides in the organism’s capsule resist host gastric acid attack, and further trigger the release of host cytokines, such as tumor necrosis factor (TNF) and interleukins-8 and interleukin-6. V. vulnificus infection blocks complement activation as well as inhibits opsonization, both necessary for bacterial eradication. Capsular polysaccharides are also are implicated in neutrophil and macrophage dysfunction. Surface pili facilitate the attachment to host cells. Flagellar elements (FHPs) are required for the development of Vibrio biofilm. Biofilm development is essential for V. vulnificus’s cytotoxicity as well as environmental survival. V. vulnificus lipopolysaccharides mediate septic shock through the release of cytokines and pyrogens.
Iron uptake during host invasion enhances the cytotoxicity and virulence of V. vulnificus. Specific metabolic pathways can strip host transferrin of iron, triggering sepsis and elevating mortality. At special risk are patients with elevated iron stores, e.g., sickle cell anemia, chronic liver disease, and hemochromatosis.
Transmission
You can get sick from Vibrio vulnificus in two ways:
- You can get infected by getting seawater on an open wound, cut, sore, or puncture. The bacterium can enter through the break in the skin and cause infection. In some people the infection heals by itself, while in others it progresses to severe infection of the skin and underlying tissues.
- You can also get sick from Vibrio vulnficus by eating raw or undercooked shellfish.
In Queensland, the majority of cases occur following exposure to the bacterium through cuts and abrasions, rather than through eating affected seafood.
There is no evidence of person-to-person transmission of Vibrio vulnificus.
Symptoms Vibrio Vulnificus
- Diarrhea and abdominal pain
- Fever, chills
- Very low blood pressure
- Blistering, warm, swollen, and reddened skin near where the bacteria entered. There can be bleeding and discharge associated with these blisters.
Vibrio Vulnificus risk factors
While not potentially life-threatening to most healthy people, symptoms of V. vulnificus infection may occur within 24 to 48 hours of ingestion and may include sudden chills, fever, nausea, vomiting, diarrhea, shock, and skin lesions. In people with certain medical conditions such as cancer, diabetes, or liver disease death can occur within two days. Anyone showing signs of any of these symptoms after eating raw oysters should seek medical attention immediately.
Certain health conditions put people at high risk for serious illness or death from V. vulnificus infections. Some of these health conditions may be present without any symptoms so people may not know they are at risk. Individuals should check with their doctors if they are unsure of their risk. Vibrio vulnificus infections in high-risk individuals have a 50 percent fatality rate.
These conditions include:
- Liver disease (from hepatitis, cirrhosis, alcoholism, or cancer)
- Iron overload disease (hemochromatosis)
- Diabetes
- Cancer (including lymphomas, leukemia, Hodgkin’s disease)
- Stomach disorders
- Or any illness or medical treatment that weakens the body’s immune system, including HIV infection
Complications
The major complications of V. vulnificus infection are sepsis, necrotizing fasciitis, myonecrosis, and extremity gangrene. The latter frequently ending in amputation.
Necrotizing fasciitis is a severe life-threatening infection of the soft tissues, involving subcutaneous fat, contiguous fascial sheets, and potentially underlying musculature.
The latter is defined as myonecrosis. Necrotizing fasciitis is frequently blamed on ‘flesh-eating bacteria’ in the lay literature. The limbs are the most frequent anatomic location, but occasionally the perineum is involved.
Underlying diabetes, hepatic disease, malignancy, intravenous drug abuse, and immunosuppression are all risk factors for its development.
Rarer complications of V. vulnificus include meningoencephalitis, peritonitis, and pneumonitis.
Diagnosis
A clinician may suspect vibriosis if a patient has watery diarrhea and has recently eaten raw or undercooked seafood, especially oysters, or when a wound infection occurs after exposure to seawater. Infection is diagnosed when Vibrio bacteria are found in the stool, wound, or blood of a patient who has symptoms of vibriosis.
Treatment for Vibrio Vulnificus
Treatment is not necessary in mild cases, but patients should drink plenty of liquids to replace fluids lost through diarrhea. Although there is no evidence that antibiotics decrease the severity or duration of illness, they are sometimes used in severe or prolonged illnesses.
Antibiotics are necessary to eradicate the infection. In case of wound infection, aggressive debridement is necessary to remove necrotic tissue. If the patient is in shock, perform the necessary interventions to resuscitate the patient. V vulnificus is the etiologic agent of necrotizing fasciitis, so we need emergency approaches to treat potential septic shock and multiple organ failure, particularly in those with preexisting medical complications, including hypotension, lactic acidosis, coagulation disorders, and thrombocytopenia.
Antibiotics are necessary to eradicate V. vulnificus infection. Effective antibiotics may include tetracycline, third-generation cephalosporins, and imipenem.
Doxycycline (Doryx, Vibramycin, Bio-Tab)
Doxycycline is a synthetic antibiotic derived from tetracycline. It inhibits protein synthesis and the bacterial growth by binding to 30S and possibly 50S ribosomal subunits of susceptible bacteria. Doxycycline is effective against a large number of pathogens.
Prevention
General recommendations for avoiding Vibrio vulnificus gastrointestinal illness and severe infection in susceptible individuals:
- Thoroughly wash hands, utensils, and surfaces after preparing or handling raw seafood.
General recommendations for avoiding wound infections:
- Do not handle raw seafood of any kind if you have a pre-existing wound.
- Wear protective clothing (ie. Gloves) when handling raw seafood.
- Avoid marine, estuarine or brackish (sea/ocean) water if you have a pre-existing wound.
- If you sustain a wound or injury while exposed to salty seawater or while handling seafood, thoroughly clean and disinfect the area immediately and seek medical attention if the area becomes inflamed.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.