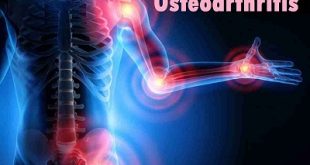
Overview of Osteogenesis Imperfecta
Osteogenesis imperfecta (OI) is a genetic disorder of connective tissues caused by an abnormality in the synthesis or processing of type I collagen (the protein that is responsible for bone structure). It is also called brittle bone disease. It is characterized by an increased susceptibility to bone fractures and decreased bone density. Other manifestations include blue sclerae, dentinogenesis imperfecta, short stature, as well as deafness in adulthood. There are also reports of valvular insufficiencies and aortic root dilation. Milder manifestations include generalized laxity, easy bruising, hernias, and excess sweating. Clinical manifestations range from mild with a nearly asymptomatic form to most severe forms (involving infants presenting with crumpled ribs, fragile cranium, and long bone fractures incompatible with life), resulting in increased perinatal mortality.
Epidemiology
The estimated incidence is approximately 1 per 20,000 live births. Persons with OI caused by collagen mutations have 50% risk of having an affected child. The proportion of cases caused by a de novo mutation varies by disease severity: they include approximately 60% of cases of classic non-deforming OI with blue sclerae or common variable OI with normal sclerae, virtually 100% of perinatally lethal OI, and close to 100% of progressively deforming OI are denovo mutations. The inherited recessive disorder is less at 25% affection; however, it is more serious.
Types of Osteogenesis Imperfecta
At least eight different forms of osteogenesis imperfecta exist, ranging in severity from a lethal form to a milder form with few visible symptoms. The specific medical problems children encounter depend on the degree of severity.
Up to 95 percent of OI cases fall into four major types of the condition:
Type I – Mild
Type I is the most common form of osteogenesis imperfecta and it’s usually inherited. Children who have Type I osteogenesis imperfecta typically don’t develop bowing deformities in the arms or legs (these are known as long bones), and their height is usually normal.
Common characteristics of children who have Type I osteogenesis imperfecta include:
- Bones that fracture more easily than normal, most often before puberty.
- A near-normal or slightly short stature.
- Whites of the eye (also known as sclera) that are blue or blue-gray.
- Dental problems (also known as dentinogenesis imperfecta).
- Hearing loss beginning around age 20 to 30.
- A curved spine.
- A triangular-shaped face.
Blue or blue-gray eye
Type II – Extremely Severe/Lethal
Children who have Type II osteogenesis imperfecta are born with severe skull, spine, chest-wall and long-bone deformities that develop as they grow in the uterus. Survival past infancy is rare. Usually a new gene mutation not an inherited gene mutation—causes osteogenesis imperfecta Type II.
Type III – Severe, Progressive Deformity
Children who have Type III osteogenesis imperfecta are born with fractures that cause moderate to severe abnormalities. X-rays might show healing fractures that happened before birth. With growth, further abnormalities develop, leading to limb shortening and bowing. These problems impair upper-extremity motion and are often severe enough that children can’t stand. Children who have Type III osteogenesis imperfecta usually have no family history of the condition.
Children with osteogenesis imperfecta Type III typically have:
- Bones that fracture more easily than normal.
- Severe hearing loss.
- Loose joints and poor muscle development in the arms and legs.
- A barrel-shaped rib cage.
- Short stature.
- A curved spine.
- A triangular-shaped face.
- Dental problems.
- Blue-gray or blue sclera.
Type IV – Moderate to Severe
Although fractures are common for children with Type IV OI, bone deformities are usually not as severe. Type IV is more severe than Type I, but not as severe as Types II or III. Type IV often can be traced through family lines.
Common characteristics of children who have Type IV include:
- Bones that fracture easily, most often before puberty.
- Normal or near-normal colored sclera.
- A curved spine.
- Loose joints.
- Short stature.
- Mild to moderate bone abnormalities.
- Hearing loss.
- A barrel-shaped rib cage.
- A triangular-shaped face.
In some cases, children who have Type IV osteogenesis imperfecta have dental problems.
Pathophysiology
The pathophysiology of osteogenesis imperfecta is primarily due to a dysfunction in collagen and is classified under connective tissue diseases.
The COL1A1 and COL1A2 gene contains instructions for creating type I collagen. Collagen is a necessary protein that provides strength to multiple tissues in the body. Type I collagen is specifically found in bone, cartilage, tendon, skin, and the many ocular tissues such as trabecular meshwork, optic nerve, sclera, and uveoscleral pathway. It is also the most abundant form of collagen in the body.
Collagen is created from procollagen, which is made of three chains. Triple stranded procollagen molecules are exported out of the cell and processed by multiple enzymes and cofactors to create the final mature collagen. Collagen strands then arrange themselves into long, thin fibrils with cross-linking to form a strong meshwork. Type I collagen is made up of two pro-α1(I) chains and one pro-α2(I) chain. COL1A1 mutations cause aberrant pro-α1(I) chains to form, whereas COL1A2 creates an aberrant pro-α2(I) chain. Therefore, poor procollagen formation yields an equally weak type I collagen to form throughout the body.
CRTAP gene (3p22.3) and P3H1/LEPRE1 (1p34.2) contain the instructions for making cartilage associated protein and enzyme prolyl-3-hydroxylase, respectively. Mutations in either gene cause problems in the normal protein folding, assembly, and secretion of the procollagen molecules resulting in weakened connective tissue and ultimate bone abnormalities, deformities, and short stature. CRTAP and P3H1 cause the rare, more severe types of OI – CRTAP gene mutations can cause type VII and P3H1 mutations cause type VIII.
Causes of Osteogenesis Imperfecta
Osteogenesis imperfecta isn’t caused by too little calcium or poor nutrition. The most common forms of OI are caused by a mutation on collagen genes. The mutation affects the body’s production of the collagen found in bones and other tissues. Other types of osteogenesis imperfecta are caused by a mutation of the cartilage-associated protein gene.
Signs and symptoms of osteogenesis imperfecta
The main sign of osteogenesis imperfecta (OI) is bones that break easily, often for no obvious reason. But the signs and symptoms of OI vary among children, and this variability includes how often their bones break.
Other signs of OI include:
- Bones that don’t grow properly or bend out of shape
- A barrel-shaped ribcage
- Scoliosis
- A blue, grey or purple tint to the sclera
- Brittle or discoloured teeth
- A triangle-shaped face
- Short stature
- A large head
- Skin that bruises easily
- Low muscle tone
- Loose joints
- Hearing problems
- Heart murmurs
A baby with OI
Possible Complications
Complications are largely based on the type of OI present. They are often directly related to the problems with weak bones and multiple fractures.
Complications may include:
- Hearing loss (common in type I and type III)
- Heart failure (type II)
- Respiratory problems and pneumonias due to chest wall deformities
- Spinal cord or brain stem problems
- Permanent deformity
Osteogenesis Imperfecta risk factors
Risk factors are details about a person that may increase the chances that they develop a specific disease or disorder.
- Heredity is the greatest risk factor. If one parent has osteogenesis imperfecta, a child has a 50 percent chance of having the condition. The most common forms of osteogenesis imperfecta are inherited and can usually be traced through the family. Less common forms are passed to children through recessive inheritance.
- Being overweight increases the risk for many health problems, such as diabetes and heart disease. Extra weight also adds stress to the bones, which is especially unhealthy for people with OI.
- Environmental factors can involve chemical exposure in the workplace.
- Behavior risk factors can include diet, alcohol consumption habits, and whether or not a person smokes.
Diagnosis
OI is often inherited from an affected parent. The diagnosis of OI is made on the basis of family history and/or clinical presentation. Frequent fractures, short stature, a blue hue to the white part of the eye (blue sclera), teeth problems (dentinogenesis imperfecta) and hearing loss that progresses after puberty may be present.
X-rays are also used to diagnose OI. X-ray findings include fractures that are at different stages of healing; an unexpected skull bone pattern called Wormian bones; and bones in the spine called “codfish vertebrae.”
Laboratory testing for OI may include either biochemical testing or DNA-based sequencing of COL1A1 and COL1A2.
- Biochemical testing involves studying collagens taken from a small skin biopsy. Changes in type I collagen are an indication of OI.
- DNA sequencing of COL1A1and COL1A2 is used to identify the type I collagen gene mutation responsible for the altered collagen protein. DNA testing requires a blood sample for DNA extraction.
Both tests are relatively sensitive, detecting approximately 90 percent and 95 percent, respectively, of individuals with the clinical diagnosis of OI. Normal biochemical and molecular testing in a child with OI warrants additional testing of less common collagen genes (CRTAP and P3H (LEPRE1)) responsible for some of the rare recessive forms of OI.
Treatment for Osteogenesis Imperfecta
The goal of treatment is to increase bone strength and help people with OI live more independently. Osteogenesis imperfecta treatment may include:
- Occupational therapy (OT): OT addresses fine motor skills, such as buttoning your shirt or tying your shoes.
- Physical therapy (PT): Physical therapists prescribe exercises that increase strength, flexibility and range of motion.
- Assistive devices: Aids such as walkers, canes or crutches can improve mobility.
- Oral and dental care: OI can lead to tooth chipping, color changes or decay. People with the condition need regular dental checkups.
- Medications: Depending on your symptoms, your provider may prescribe medicines that slow bone loss or treat pain.
What is the treatment for broken bones?
If you or your child breaks a bone, an orthopedic specialist (bone specialist) can treat it. Treatment may include:
- Braces, splints or casts: An orthopedic specialist may use protective devices to stabilize broken bones during healing or after surgery.
- Surgery: Your provider may operate to correct curved or misshapen bones. Rodding surgery is a common treatment for children with OI. It uses a rod to prevent bones from breaking. The rods also support bones. Some types can be adjusted as your child grows.
How to prevent osteogenesis imperfecta?
Since this is a genetic disorder, there isn’t much an individual can do to prevent osteogenesis imperfecta. However, light exercise and low impact physical activity are suggested.
How to help a child living with osteogenesis imperfecta?
OI is a lifelong condition. Managing it may include:
- Preventing fractures. If your baby has medium to severe OI, they need to be picked up, diapered, and dressed very carefully. Their position should be changed throughout the day. As your baby gets older, it will be important to help them avoid injuries. A physical or occupational therapist, as well as other healthcare providers, can help.
- Preventing infection. Your baby may be more likely to get colds and other respiratory infections. And they may get sicker with an infection. Make sure your baby has all of their advised vaccines (immunizations). During cold and flu season, keep your child away from crowds. Make sure that you wash your hands and your child’s hands well. As your child gets older, teach them how to do it.
- Managing pain. Fractures and deformities can be very painful. Talk with your baby’s healthcare provider about pain medicine or other ways to lessen pain.
- Coping with challenges. As your child gets older, they may have emotional and physical challenges.
- Getting regular medical and dental checkups. Your baby will need regular checkups and tests. These include eye and dental exams.
- Managing weight. When your child gets older, they may gain weight because of the decreased physical activity.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.