Definition
Leukodystrophies are a group of disorders that cause deterioration of the white matter, or myelin, in the brain. The term Leukodystrophy is derived from the prefix leuko, meaning white, and the word dystrophy, meaning imperfect growth. Therefore, Leukodystrophies are characterized by imperfect growth of the white matter in the brain.
Types of Leukodystrophy
Some of the many different types of leukodystrophy include:
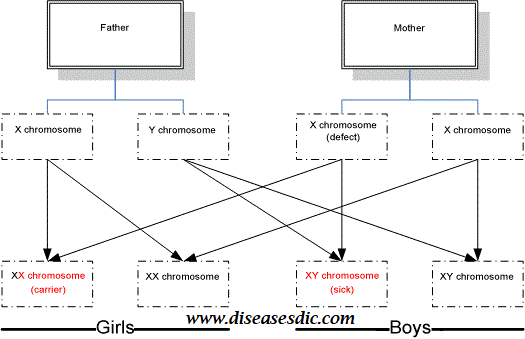
Adrenoleukodystrophy (ALD) – this is one of the more common of the leukodystrophies. Typically, it only affects boys. It is due to an X-linked gene. Symptoms of the childhood cerebral form usually begin before 10 years of age and may progress rapidly. The adrenal glands may also be affected, which means not enough cortisone is produced. The same genetic change can lead to adrenomyeloneuropathy in adults. This form affects the spinal cord and the adrenal glands. Female carriers of the gene may show similar, but usually much milder, symptoms. In some with the same genetic change, the adrenal gland may be affected in isolation.
Metachromatic leukodystrophy (MLD) – this is another common leukodystrophy. It has a range of subtypes, some of which relate to the age when symptoms appear – for example, late infantile MLD, juvenile MLD and adult MLD. In the infantile form, a loss of motor (movement) and verbal skill may be the first signs. Symptoms typically become progressively worse.
Canavan’s disease (spongy degeneration) – this form causes abnormal myelin growth. The typical form is characterised by poor head control, decreased tone, regression and a markedly enlarged head. Eventually, the decreased tone changes to stiffness. Life expectancy is limited.
Krabbe disease (globoid leukodystrophy) – this affects the myelin of the central and peripheral nervous systems. About 90 per cent of those affected are babies, and symptoms usually show up before they are six months old. There is also a rare adult form.
Pathophysiology
A majority of leukodystrophies are monogenetic disorders, affecting the gene that usually encodes a protein or an enzyme that maintains neuronal health and is responsible for regulating brain metabolism. As many of these enzymes play a role in lipid metabolism, the ineptitude to synthesize or degrade a substrate leads to a downstream lack or an upstream excess of vital lipids.
This can in turn result in a wide array of pathologies – from inflammatory demyelation, to the degeneration of axons and activation of microglia. Therefore, the aforementioned demyelination or hypomyelination are only one manifestation seen in leukodystrophies, as the myelinating oligodendrocytes are not the only cells affected in these conditions.
The major leukodystrophy disorders involve abnormal transport or degradation of myelin and oligodendrocyte sphingolipids, or of the myelin proteins. The abnormal processing of the metabolites can take place in the lysosome, at the peroxisome level, or can affect adequate functioning of mitochondria.
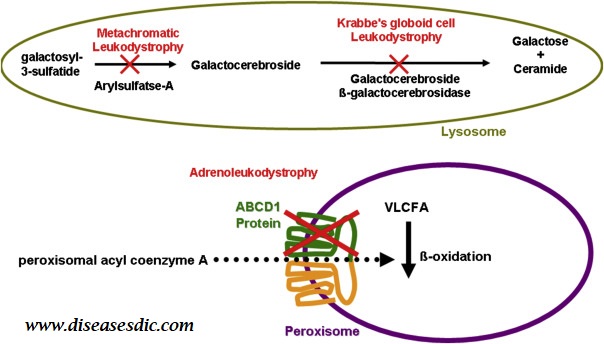
Examples of lysosomal disorders include metachromatic leukodystrophy, globoid cell leukodystrophy or Krabbe disease, and various mucolipidoses and gangliosidoses. X-linked adrenoleukodystrophy is a peroxisomal disorder, while spongiform leukodystrophy (Canavan disease) and trichopoliodystrophy (Menkes syndrome) affect the mitochondria.
Causes and Risk factors
Leukodystrophies are genetic disorders caused by specific gene abnormalities that lead to abnormal development or destruction of the myelin sheath in the nervous system or white matter in the brain. Each type of leukodystrophy follows a particular pattern of inheritance such as autosomal recessive, X-linked recessive or autosomal dominant.
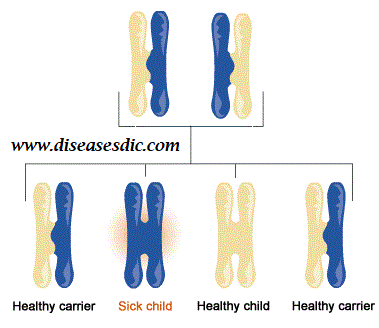
There are some leukodystrophies that do not appear to be inherited, but rather arise spontaneously. They are still caused by a mutation in a particular gene, but it means that the mutation was not inherited. In this case, the birth of one child with the disease does not necessarily increase the likelihood of a sibling having the disease. A family history of leukodystrophy may increase your chance of leukodystrophy.
Signs and symptoms
Symptoms of leukodystrophies vary by disease, progression and the areas of the brain affected. Some common symptoms include:
- Developmental regression (loss of skills previously achieved)
- Trouble with motor skills such as new onset problems with walking
- Seizures
- Cognitive decline
As the disease progresses, symptoms can include:
- Abnormal body and muscle tone
- Abnormal movements
- Increased difficulty or loss of ability to walk
- Trouble with speech
- Difficulty with eating
- Decline in vision and/or hearing
- Decline in mental and physical development
Specific symptoms will vary according to the type of leukodystrophy your child has and how much the disease has progressed. Also, each leukodystrophy can affect a child in a unique way. You can work with your care team to discuss what specific concerns you have regarding your child.
Complications
Many patients have preserved cognitive skills, at least in the beginning of the disease. Over time, depending on the type of leukodystrophy, other medical complications may develop, to include problems with chewing and swallowing, digestion and gastro-esophageal reflux (or heart burn), breathing and sleeping problems. Some, but not all, patients may have seizures.
Some leukodystrophies progress rapidly, with changes in patient health and well-being over the course of month, while other leukodystrophies progress only very slowly if at all, with changes measured in years or even decades.
Diagnosis and Screening
You will be asked about your symptoms and medical history. A physical exam will be done.
Images of the brain may be taken. This can be done with:
- MRI scan
- CT scan
Your bodily fluids and tissues may be tested. This can be done with:
- Urine analysis
- Nerve or brain biopsy
- Blood tests, which include genetic testing
- Lumbar puncture
Tests may be done on your nerves. This can be done with:
- Nerve conduction testing
- Evoked potential test
In rare cases, a brain biopsy may be done.
Treatment and Medications
Currently, leukodystrophies cannot be cured. Stem cell therapy and bone marrow transplantation have each been tried in some cases. However, the benefits depend on the timing, age of onset and severity of symptoms. Therapies such as gene therapy and enzyme replacement therapy are under investigation. Treatment is mainly supportive and may include:
- Physical therapy
- Occupational therapy
- Psychological counselling
- Family counselling (including genetic counselling)
- Medications (for example, medications for seizures).
Prevention
There is no known way to prevent leukodystrophy. For parents who have had a child with leukodystrophy, genetic counseling may be helpful. This counseling will help to determine the chances of having another child with the disease.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.







