Definition
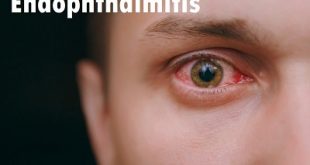
Blepharitis is a very common inflammatory disorder of the edge of the eyelids where the eyelashes are located. Bacteria, which normally exist on our skin, are drawn to crusts around the base of the eyelashes and produce chemical substances which irritate the eyes resulting in itching, irritation and burning of the eyes. The ducts of special glands, called meibomian glands, which are located in the eyelids just behind the eyelashes, become blocked. These glands are important in helping to prevent the film of tears which covers the very sensitive cornea (the clear window of the eye) from evaporating too rapidly in between blinks, as they produce the mucus layer of the tear film.
It results in:
- Tear film instability which in turns results in irritation, a foreign body sensation, burning, itching and redness of the eyes (dry eye symptoms)
- Tearing of the eyes due to an overproduction and overflow of tears as a reflex reaction to eye irritation
- Red inflamed eyelid margins
- Cyst formation in the eyelid (chalazion or meibomian cyst – see photograph below)
- Loss of eyelashes
- Inturning of the eyelid margins (entropion) resulting in painful rubbing of the eyelashes against the cornea
- Corneal ulcer (marginal ulcer or marginal keratitis)
Prevalence
It is one of the most common ocular disorders encountered by eye care practitioners. In the United States, blepharitis is estimated to affect more than 180 million people. In a United States survey of ophthalmologists and optometrists, it was estimated that 37% and 47% of the patients presented with certain form of blepharitis in clinical practice, respectively.
Blepharitis
Types of Blepharitis
Anterior blepharitis
Anterior blepharitis is the name given to the condition when the inflammation affects the skin around the base of the eyelashes.
Anterior blepharitis is usually caused by one of two things.
- Seborrhoeic dermatitis. This complaint causes the skin to become oily or flaky, blocking the Meibomian glands in the eyelid.
- A reaction to Staphylococcus bacteria, which is usually present but harmless on our skin.
Posterior blepharitis
In patients with posterior blepharitis, the inflammation usually affects the Meibomian glands which are behind the base of the eyelashes. Posterior blepharitis is normally caused by issues with the Meibomian glands, such as when they become blocked by flakes of skin, debris or bacteria. Occasionally, people who suffer from the skin condition known as Rosacea, will also find they are prone to posterior blepharitis.
Mixed blepharitis
Unsurprisingly, mixed blepharitis is a combination of both anterior and posterior types of the condition.
Risk factors
A risk factor is something that increases your chance of getting a disease or condition. Risk factors for blepharitis include:
- Seborrheic dermatitis
- Acne rosacea
- Contact allergies
- Diabetes
- Chemical irritants
- Poor hygiene
- Cosmetic makeup
- Advanced age
Causes of Blepharitis
There are a number of possible causes of blepharitis.
They include:
- An inflammatory reaction to bacteria that normally live on eyelids
- Seborrheic dermatitis or rosacea
- Parasites: Demodex eyelash mites
- Infection with the herpes simplex virus (HSV)
People who have dandruff are more likely to develop blepharitis. Keeping the dandruff under control can help reduce the symptoms.
Another possible cause is dysfunction of the Meibomian glands on the rim of the eyelids. These glands produce an oily substance that prevents the eye’s film of tears from evaporating.
Some doctors believe that blepharitis is a precursor of Meibomian gland dysfunction, rather than the gland dysfunction causing blepharitis.
Blepharitis symptoms
Blepharitis causes varying degrees of discomfort depending on the severity of the case. Common signs and symptoms include:
- Itchy, flaky eyelid margins
- Red/blood-shot eyes
- Foreign body sensation
- Excessive or frothy tears
- Crusty or sticky lashes
- Sensitivity to light
- Rough, scaly eyelids
- Excessive blinking
It is a good idea to make an appointment with your optometrist or ophthalmologist as soon you experience any of the above symptoms.
Symptoms of Blepharitis
Complications of Blepharitis
It is unusual for blepharitis to cause serious medical problems. However, blepharitis can lead to the following changes in eye health.
Sty: A sty (sometimes spelled stye) or hordeolum is a bacterial infection in one of the oil glands whose opening is clogged. The result is a painful lump on the edge or inside of the eyelid.
Chalazion: A chalazion or conjunctival granuloma occurs when blockage in one or more of the oil glands causes it/them to become enlarged and scarred. Multiple chalazia can also develop, either on the same eyelid or on different lids.
Chronic pinkeye: Blepharitis can lead to recurrent bouts of pinkeye (conjunctivitis).
Ulceration of the cornea: Constant irritation from inflamed eyelids or misdirected eyelashes may cause a sore (ulcer) to develop on the cornea. It does not affect vision generally, although disturbances of the tear film may intermittently blur vision, causing varying amounts of fluctuating vision during the day.
Diagnosis and test
Blepharitis can be diagnosed through a comprehensive eye examination. Testing, with special emphasis on the eyelids and front surface of the eyeball, may include:
- Patient history to determine any symptoms the patient is experiencing and any general health problems that may be contributing to the eye problem.
- External examination of the eye, including lid structure, skin texture and eyelash appearance.
- Evaluation of the lid margins, base of the eyelashes and meibomian gland openings using bright light and magnification.
- Evaluation of the quantity and quality of tears to check for any abnormalities.
An optometrist can determine the type of blepharitis based on the appearance of the eyelid margins. The different types and symptoms are as follows:
- Staphyloccal blepharitis patients frequently exhibit mildly sticking eyelids, thickened lid margins, and missing and misdirected eyelashes.
- Seborrheic blepharitis patients have greasy flakes or scales around the base of eyelashes and a mild redness of the eyelids.
- Ulcerative blepharitis patients have matted hard crusts around the eyelashes. Removing the crusts leaves small sores that ooze and bleed. These patients may also experience eyelash loss, distortion of the front edges of the eyelids and chronic tearing. In severe cases, the cornea (the transparent front covering of the eyeball) becomes inflamed.
- Meibomian blepharitis patients have a blockage of the oil glands in the eyelids, poor quality of tears and redness of the lining of the eyelids.
Treatment and medications
Blepharitis cannot be totally cured, but it is possible to make your eyes more comfortable:
Warm compresses- These will help to unblock glands and loosen the crusts on the eyelid so that they are easier to remove. You can buy reusable warming packs which you heat up in the microwave, or you can use a flannel, cotton-wool ball or something similar, which you can soak in hot, but not boiling, water. Place the compress on the edge of your closed eyelids for five minutes, rocking it gently. This will loosen the crusts. Use a use a separate clean compress for each eye.
Lid cleaning- After applying the compress you should clean your lids. Your optometrist will be able to advise you of the different options available.
Lubricants- These are available from your optometrist or pharmacist and can help if your eyes feel gritty and dry.
Antibiotics- If warm compresses and cleaning your eye lids do not work, your doctor or prescribing optometrist may prescribe you antibiotic ointment or tablets. You may need to take these for several weeks or months and the benefits may last for some months after you finish the treatment.
If you have blepharitis, avoid smoky atmospheres and wearing eye makeup, particularly eyeliner and mascara.
Prevention
- Strict eye hygiene helps prevent blepharitis. Using clean towels and making sure your hands are clean before touching your eyes and eye area are important steps in prevention. If you wear makeup, it is important to thoroughly remove any traces of it before going to bed.
- In cases of posterior blepharitis where the oil glands are not producing enough oil, nutritional supplements of Omega-3 fatty acids may be recommended by your doctor. Flaxseed oil is a common fatty acid supplement.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.