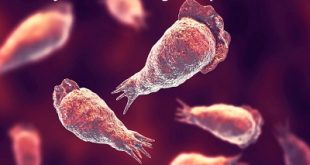
What is melioidosis?
Melioidosis, also known as Whitmore’s disease, is an uncommon bacterial infection caused by Burkholderia pseudomallei. The disease affects humans and animals. Individuals acquire the bacteria through direct contact with contaminated soil and surface waters.
Transmission
The bacterium that causes melioidosis usually enters the body via cuts and sores in the skin, or via inhalation of dust or droplets, and very rarely by ingestion of contaminated water. Melioidosis does not usually spread from one person to another or from animals to humans.
During the dry season the bacterium is found in deeper soil layers, but during the wet season it can be found in the surface layers and in muddy surface waters. This is why most cases of melioidosis occur during the wet season following heavy rains and flooding.
Causes
A person can get melioidosis when they come into contact with water or soil that carries the bacterium Burkholderia pseudomallei.
This can happen if a person:
- Comes into contact with contaminated soil, especially via skin cuts or abrasions
- Drinks contaminated water
- Inhales dust or water droplets
Human-to-human transmission is. However, it is possible for a person to transmit the bacterium to another person.
What are risk factors for melioidosis?
Risk factors for developing melioidosis infection include
- Living in Southeast Asia and northern Australia
- Diabetes
- Alcohol abuse
- Chronic renal disease
- Chronic lung disease
- Liver disease
- Thalassemia
- Kava consumption
- Cancer or another immune-suppressing condition not related to HIV, and
- Chronic lung disease (such as cystic fibrosis, chronic obstructive pulmonary disease or (COPD), and bronchiectasis)
Other possible risk factors that may contribute to infection with melioidosis include steroid and other immunosuppressive therapy, rheumatic heart disease, congestive heart failure, pulmonary hemosiderosis, chronic granulomatous disease, and tuberculosis.
Signs and Symptoms
Melioidosis has a wide range of signs and symptoms. It can be mistaken for other diseases, such as tuberculosis or more common forms of pneumonia.
There are several types of melioidosis infection, each with their own set of symptoms.
Localized Infection:
- Localized pain or swelling
- Fever
- Ulceration
- Abscess
Pulmonary Infection:
- Cough
- Chest pain
- High fever
- Headache
- Anorexia
Bloodstream Infection:
- Fever
- Headache
- Respiratory distress
- Abdominal discomfort
- Joint pain
- Disorientation
Disseminated Infection:
- Fever
- Weight loss
- Stomach or chest pain
- Muscle or joint pain
- Headache
- Central nervous system/brain infection
- Seizures
The incubation period for melioidosis (time between exposure to the bacteria that causes the disease and the appearance of symptoms) is not clearly defined. It can range from one day to many years, but generally symptoms appear two to four weeks after exposure.
What are the complications of melioidosis?
Melioidosis can be life-threatening. The risk is increased with:
- More extensive or severe disease
- Comorbidities such as chronic diseases (diabetes, chronic lung disease, the liver or kidney disease) or immunosuppression.
Complications of melioidosis include:
- Sepsis
- Organ failure
- Pneumothorax (collapsed thorax)
- Cardiac tamponade (fluid buildup in the pericardial area)
- Recurrence of infection.
Melioidosis Diagnosis
Your doctor can diagnose a melioidosis infection by separating Burkholderia pseudomallei bacteria from:
- Blood test
- Urine sample
- Throat swab
- Skin lesion test
- Abscesses
Doctors may also diagnose it by looking for an antibody response to the bacteria.
They may identify the diagnosis as:
- Localized infection — it’s limited to one part of the body.
- Lung infection
- Bloodstream infection
- Disseminated infection — the bacteria may have spread to different organs in the body.
Treatment
When a melioidosis infection is diagnosed, the disease can be treated with the use of appropriate medication.
The type of infection and the course of treatment will impact long-term outcome. Treatment generally starts with intravenous (within a vein) antimicrobial therapy for a minimum of 2 weeks (up to 8 weeks depending on extent of infection), followed by 3–6 months of oral antimicrobial therapy.
Intravenous therapy consists of:
- Ceftazidime administered every 6–8 hours (or)
- Meropenem administered every 8 hours
Oral antimicrobial therapy consists of:
- Trimethoprim-sulfamethoxazole taken every 12 hours
- Amoxicillin/clavulanic acid (co-amoxiclav) taken every 8 hours
Patients with penicillin allergies should notify their doctor, who can prescribe an alternative treatment course.
How to prevent melioidosis?
There are no vaccines for humans to prevent melioidosis, though they are being studied.
People who live in or are visiting areas where melioidosis is common should take these actions to prevent infection:
- When working in soil or water, wear waterproof boots and gloves.
- Avoid contact with soil and standing water if you have open wounds, diabetes, or chronic kidney disease.
- Be vigilant about avoiding exposure by inhalation during severe weather events.
- Healthcare workers should wear masks, gloves, and gowns.
- Meat cutters and processors should wear gloves and regularly disinfect knives.
- If drinking dairy products, be sure they are pasteurized.
- Get screened for melioidosis if you’re about to start immunosuppressive therapy.
 Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.
Diseases Treatments Dictionary This is complete solution to read all diseases treatments Which covers Prevention, Causes, Symptoms, Medical Terms, Drugs, Prescription, Natural Remedies with cures and Treatments. Most of the common diseases were listed in names, split with categories.